Coconut oil is often hailed for its moisturizing and soothing properties, but when it comes to sunburn relief, opinions vary. While it’s tempting to reach for coconut oil due to its natural appeal, it’s important to understand its potential effects on sunburned skin. Sunburn causes skin to become inflamed, red, and painful, which can make it sensitive to various treatments. Although coconut oil may offer hydration, it can also trap heat if applied too soon, potentially worsening the discomfort. This article explores whether coconut oil is an effective remedy for sunburn and how it interacts with the healing process of damaged skin.
What a sunburn actually is and what your skin needs first:

A sunburn is your skin’s inflammatory reaction to UV damage. The upper layers of skin lose water, the barrier becomes “leaky,” and nerve endings become more sensitive—so you feel heat, pain, tightness, and later, peeling.
Think of it like this: your skin is an overheated roof that’s started leaking. The first job isn’t to “seal” it with something heavy—it’s to cool it down and replenish water, then support barrier repair.
Dermatology organizations commonly recommend:
- cool baths/showers or cool compresses
- moisturizer with aloe vera or soy (applied while skin is damp)
- anti-inflammatory pain relief (if you can take it)
- extra hydration and sun avoidance while healing
Who may benefit from coconut oil:
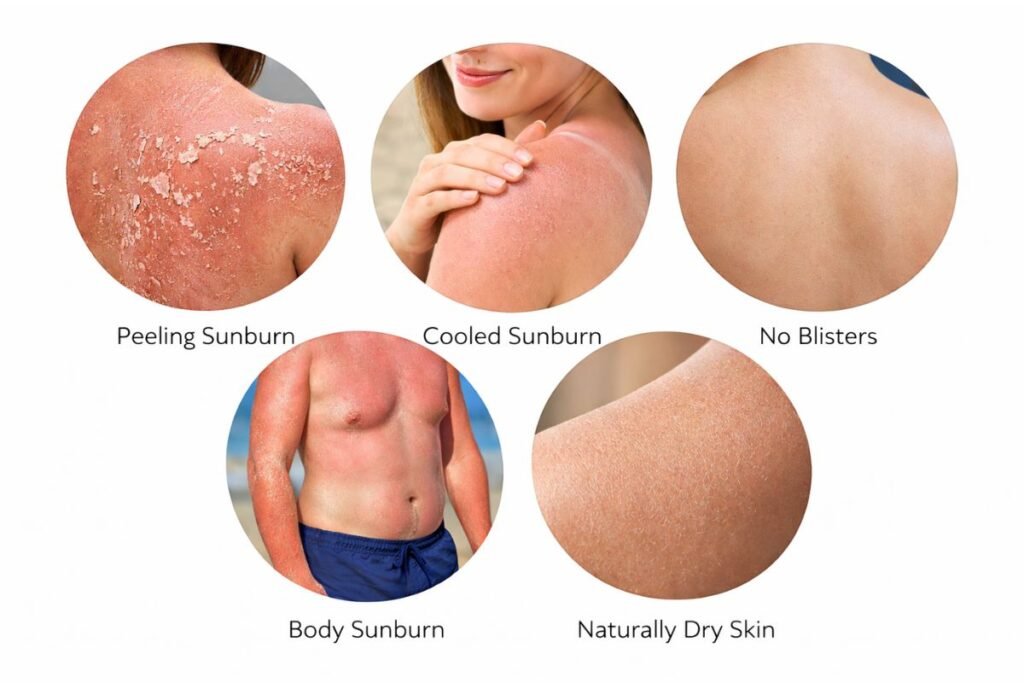
You may benefit if:
1) Mild sunburn in the dry/peeling phase:
If your burn has moved past the “hot, inflamed” stage and you’re now dealing mainly with tightness, flaking, or peeling, coconut oil may help by softening rough patches and reducing visible dryness.
2) Skin that’s no longer hot or throbbing:
Coconut oil is best considered only when the skin feels cool and calm. When skin is still hot, applying a heavy oil can feel uncomfortable and may “seal in” heat.
3) Intact skin with no blisters or open areas:
Coconut oil should only be used on unbroken skin. If you have blisters, cracks, or raw areas, using oils can increase irritation and may raise the risk of infection.
4) Body sunburn (arms, legs, chest, back) rather than the face:
Body skin tends to tolerate heavier products better than facial skin. Using coconut oil on the face—especially around the T-zone—can trigger clogged pores in many people, so it’s generally safer for non-acne-prone body areas.
5) Naturally dry, non–breakout-prone skin:
If your skin is typically dry and not prone to acne, folliculitis, or bumps, coconut oil may provide a temporary comfort boost by sealing in moisture and improving softness during healing.
Who should avoid coconut oil or get medical advice first:
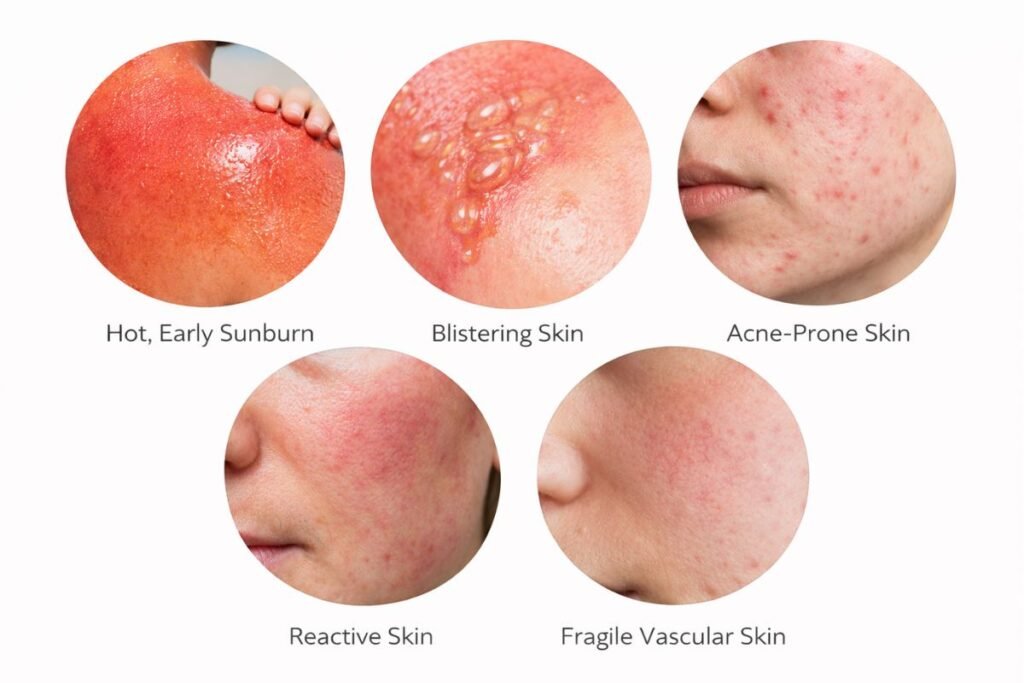
Avoid coconut oil (or get medical advice first) if you have:
1) Severe sunburn or early “hot” sunburn stage:
If your skin is bright red, burning, swollen, or painful to touch, skip coconut oil. At this stage, you’ll do better with cool compresses and lightweight, fragrance-free moisturizers.
2) Blistering, broken skin, or oozing areas:
Any sign of blistering, peeling that becomes raw, or open skin is a reason to avoid coconut oil and focus on medical-grade barrier support. These burns can require professional care.
3) Acne-prone skin or history of clogged pores:
Coconut oil can clogged pores for many people. If you break out easily, it may lead to whiteheads, bumps, or folliculitis, especially on the face, chest, or back.
4) Eczema, rosacea, psoriasis, or highly reactive skin:
If you’re prone to flares, your skin barrier is already sensitive. Coconut oil may feel too occlusive and can sometimes trigger stinging, redness, or itching. A bland, fragrance-free moisturizer is usually safer.
5) Fragile vascular skin (broken capillaries / easy flushing):
If you have visible broken capillaries or skin that flushes easily, heavy occlusives may worsen the sensation of heat and redness. Stick to lightweight soothing lotions until fully healed.
Note: Cleveland Clinic dermatology commentary mentions coconut oil can clog pores and worsen acne/comedones for some people—especially on the face and trunk.
How coconut oil works and what it can’t promise:
What it can do (more supported):
Coconut oil is primarily an emollient and occlusive:
- emollient: smooths rough, flaky skin (temporary softness)
- occlusive: slows water loss by forming a film (temporary reduction in tightness)
There is also evidence that virgin coconut oil may support barrier function in certain dry-skin conditions. Clinical trials have compared virgin coconut oil to mineral oil for xerosis (dry skin) and found it can improve dryness when used regularly. In children with mild-to-moderate atopic dermatitis, a randomized trial found topical virgin coconut oil improved disease severity measures and skin barrier metrics compared with mineral oil.
What’s limited (sunburn-specific evidence):
There isn’t strong clinical evidence that coconut oil treats acute sunburn better than standard care. Sunburn is fundamentally an inflammatory heat injury plus barrier disruption. In the early stage, sealing the skin with a heavy oil may feel suffocating and can trap heat, which is why many clinicians recommend lighter, water-based soothing options first. Public health guidance also warns against ice on sunburned skin and advises gentle cooling measures instead.
Temporary cosmetic effects vs. long-term outcomes:
- temporary: coconut oil may make peeling skin look less flaky and feel less tight for a few hours
- long-term: coconut oil does not reverse UV DNA damage, prevent long-term photoaging, or reduce skin cancer risk. Long-term protection comes from sun avoidance during healing and consistent broad-spectrum SPF afterward.
Safe frequency and where coconut oil fits in your routine:
Best timing:
- first 24–48 hours: avoid coconut oil if the skin is hot, very red, or swollen
- after the burn cools: consider coconut oil only if the skin is intact and mainly dry/peeling
How often (range):
- start once daily, then increase to 1–2 times per day as tolerated if you’re not breaking out or getting itchy
- if you’re using it over a moisturizer, you usually need less—often 2–3 nights per week is enough for many people
Where it goes (simple sunburn recovery order):
- cool shower (not hot), gently pat dry
- light moisturizer or aloe/soy lotion while skin is damp
- optional: a very thin layer of coconut oil only at night on extra-dry areas (late-stage)
Tip: Instead of straight coconut oil, mix a small amount into your fragrance-free moisturizer for a lighter feel.
Detailed risks :
Risk 1: Heat trapping and prolonged discomfort:
In early sunburn, heavy occlusives (including oils) can feel like they “seal in” heat. If your skin is still hot/red/swollen, go lighter and focus on cooling first.
Risk 2: Ice burn / cold injury:
Putting ice or ice packs directly on sunburned skin can cause additional injury. Use cool water or a cool damp cloth instead.
Risk 3: Rosacea flares and broken capillaries:
If you flush easily, have rosacea, or visible tiny vessels, heat-trapping products can worsen redness. Stick to lightweight, fragrance-free lotions and avoid heavy oils until fully calm.
Risk 4: Eczema irritation and contact dermatitis:
Coconut-derived ingredients can trigger irritation in reactive skin. Patch test first and stop if burning/itching increases.
Risk 5: Clogged pores, folliculitis, milia:
Coconut oil is comedogenic for many people and may trigger bumps, whiteheads, or acne—especially on the face, chest, back, and shoulders.
Risk 6: Blistered or broken skin complications
Blisters mean a deeper burn and a higher infection risk. Don’t pop blisters. Seek medical guidance for extensive blistering or systemic symptoms.
When to stop and what to do instead:
Stop coconut oil immediately if you notice:
- new itchy rash, hives, or stinging that worsens
- increased redness/heat after application
- new bumps, clogged pores, or pustules
- signs of infection: worsening pain, spreading redness, pus, fever
Switch to:
- a bland, fragrance-free moisturizer
- aloe/soy moisturizer for soothing (especially early)
- cool compresses and hydration
Seek urgent medical care if:
- sunburn covers a large area with blistering
- you have fever, chills, confusion, severe dehydration, or significant facial swelling
- pain is severe or worsening after 48 hours
Realistic results timeline:
Week 1–2
- pain/heat usually improves over several days
- peeling commonly begins around days 3–7
- coconut oil (if used late-stage) may temporarily reduce flaking and tightness
Month 1
- most texture changes normalize
- lingering redness or pigmentation may occur after deeper burns
Month 3
- barrier should be stable again
- if discoloration or sensitivity persists, consider a dermatologist visit
Common mistakes and how to fix them:
Mistake: Using coconut oil immediately after getting burned
Fix: use cooling and light moisturizer for 24–48 hours, then consider oil only if you’re peeling and the skin is cool and intact.
Mistake: Putting ice directly on the burn
Fix: use a cool damp cloth 10–15 minutes, repeat 2–4 times daily.
Mistake: Using numbing sprays/creams (“-caine” products)
Fix: use gentle moisturizers, cool compresses, and anti-inflammatory pain relief if safe for you; avoid products that sting or irritate.
Mistake: Scrubbing or exfoliating peeling skin
Fix: pat dry, moisturize often, and let peeling skin shed naturally.
Mistake: Restarting retinoids/acids too soon
Fix: wait until tenderness is gone and the barrier feels normal, then reintroduce slowly.
FAQs:
Can I use coconut oil on sunburn?
Yes—but timing matters. If your sunburn is still hot, bright red, swollen, or actively inflamed, avoid coconut oil for the first 24–48 hours because heavy, occlusive oils can trap heat and may worsen discomfort. Once the burn has cooled and the skin is intact (no open blisters), a thin layer may help with late-stage dryness and peeling. Evidence for sunburn-specific benefit is limited, and it can clog pores or irritate sensitive skin.
My skin feels hot and throbbing—what helps fastest?
Use cool showers or baths, apply cool compresses for 10–15 minutes (repeat 2–4 times daily), and moisturize while skin is damp using a gentle, lightweight lotion (often aloe- or soy-based). Drink extra water and avoid sun exposure while healing. Skip coconut oil in the early hot stage.
I’m peeling and itchy—can coconut oil help now?
Sometimes, yes—only if the skin is cool and intact (no blisters, cracks, raw areas, or oozing). In the dry/peeling phase, a very thin layer can soften rough patches and reduce tightness for a few hours. Start once daily (preferably at night) and stop if you get bumps, irritation, or worsening redness.
Will I get dark spots after this?
It can happen, especially in deeper skin tones. Don’t pick peeling skin. Once tenderness settles, moisturize gently and protect the area from sun exposure with consistent broad-spectrum SPF and covering up. If discoloration persists beyond a few weeks, a dermatologist can guide safe brightening options—avoid starting strong acids or retinoids too soon after a burn.
Can I use coconut oil on my face after sunburn?
Usually not ideal if you’re acne-prone or clog easily. Coconut oil can trigger clogged pores, bumps, or folliculitis—especially on the face, chest, and back. A non-comedogenic, fragrance-free moisturizer is typically safer for facial skin.
How often should I use coconut oil if I tolerate it?
Start once daily. If your skin stays calm and you don’t break out or itch, you can increase to 1–2 times daily, or use it only 2–3 nights per week over your moisturizer. Mixing a small amount into a fragrance-free moisturizer can feel lighter than applying it alone.
When should I avoid coconut oil completely?
Avoid coconut oil if:
- the sunburn is still hot, swollen, and painful
- you have blisters, open skin, or oozing
- you have acne-prone skin or a history of clogged pores
- you have eczema, rosacea, psoriasis, or highly reactive skin
- you flush easily or have fragile vascular skin (visible broken capillaries)
What’s better than coconut oil for fresh sunburn pain?
Cool showers/compresses, aloe- or soy-based moisturizers applied while skin is damp, hydration, and strict sun avoidance are usually best early on. Avoid ice directly on skin. If safe for you, anti-inflammatory pain relief may help with discomfort.
When should I seek medical care for sunburn?
Seek urgent care if you have widespread blistering, fever/chills, confusion, severe dehydration, significant facial swelling, signs of infection (spreading redness, pus, fever), or pain that is severe or worsening after 48 hours.







